Kwashiorkor
Kwashiorkor is a protein malnutrition. It is caused by protein deficiency.
Who discovered kwashiorkor?
In 1933, Cicely Williams was the first in Africa to describe kwashiorkor, the nutritional disease of childhood associated with a maize diet.
Which of the following symptoms is characteristic of kwashiorkor?
Kwashiorkor is a condition resulting from inadequate protein intake. Early symptoms include fatigue, irritability, and lethargy. As protein deprivation continues, one sees growth failure, loss of muscle mass, generalized swelling (edema), and decreased immunity.
What causes kwashiorkor?
The main cause of kwashiorkor is not eating enough protein or other essential vitamins and minerals. It’s most common in developing countries with a limited food supply, poor hygiene, and a lack of education about the importance of giving babies and children an adequate diet.
What is kwashiorkor and its symptoms?
Kwashiorkor is a condition resulting from inadequate protein intake. Early symptoms include fatigue, irritability, and lethargy. As protein deprivation continues, one sees growth failure, loss of muscle mass, generalized swelling (edema), and decreased immunity. A large, protuberant belly is common.
What deficiency causes kwashiorkor disease?
Kwashiorkor is caused by a lack of protein in the diet. Every cell in your body contains protein. You need protein in your diet for your body to repair cells and make new cells. A healthy human body regenerates cells in this way constantly.
What causes fatty liver in kwashiorkor?
Recent abservations suggest that a relative deficiency in the synthesis of beta protein, rather than a deficiency in choline for phosphatidyl choline synthesis, is the more likely cause of liver steatosis in kwashiorkor.
Is there ascites in kwashiorkor?
Children with kwashiorkor also have typical skin and hair changes (see earlier sections on hair and skin changes). The abdomen is protuberant because of weakened abdominal muscles, intestinal distention, and hepatomegaly, but these children do not have ascites.
Is kwashiorkor acute or chronic?
Marasmic kwashiorkor is caused by acute or chronic protein deficiency and chronic energy deficit and is characterized by edema, wasting, stunting, and mild hepatomegaly. The distinction between kwashiorkor and marasmus is frequently blurred, and many children present with features of both conditions.
How does kwashiorkor affect the digestive system?
Abnormalities of the gastrointestinal tract including atrophy of the pancreas with subsequent glucose intolerance, atrophy of the mucosa of the small intestine, lactase deficiency, ileus, bacterial overgrowth, which can lead to bacterial septicemia and death.
How long does it take to recover from kwashiorkor?
The overall median time of recovery was 42 days with 35 days for children with kwashiorkor and 49 days for children with marasmus.
What is the major difference to distinguish between kwashiorkor and marasmus?
Marasmus occurrence increases prior to age 1, whereas kwashiorkor occurrence increases after 18 months. It can be distinguished from kwashiorkor in that kwashiorkor is protein deficiency with adequate energy intake whereas marasmus is inadequate energy intake in all forms, including protein.
Is kwashiorkor similar to protein energy malnutrition?
Protein-energy malnutrition (PEM) is a common childhood disorder and is primarily caused by deficiency of energy, protein, and micronutrients. PEM manifests as underweight (low body weight compared with healthy peers), stunting (poor linear growth), wasting (acute weight loss), or edematous malnutrition (kwashiorkor).
Where is kwashiorkor most common in the world?
If the body lacks protein, growth and normal body functions will begin to shut down, and kwashiorkor may develop. Kwashiorkor is most common in countries where there is a limited supply or lack of food. It is mostly found in children and infants in sub-Saharan Africa, Southeast Asia, and Central America .
What is the biochemical basis of kwashiorkor?
Kwashiorkor is a severe form of malnutrition associated with a deficiency in dietary protein. The extreme lack of protein causes an osmotic imbalance in the gastrointestinal system causing swelling of the gut diagnosed as an edema or retention of water.
Can kwashiorkor occur in adults?
Kwashiorkor is rare in developed countries such as the UK, but it can occasionally happen as a result of severe neglect, long-term illness, a lack of knowledge about good nutrition, or a very restricted diet. Although kwashiorkor can affect people of all ages, it’s more common in children than adults.
How is kwashiorkor treated?
Kwashiorkor can be corrected by eating more protein and more calories overall, especially if treatment is started early.
You may first be given more calories in the form of carbohydrates, sugars, and fats. Once these calories provide energy, you will be given foods with proteins.
Foods must be introduced and calories should be increased slowly because you have been without proper nutrition for a long period. Your body may need to adjust to the increased intake.
Your doctor will also recommend long-term vitamin and mineral supplementation to your diet.
What are the complications of kwashiorkor?
Even with treatment, children who have had kwashiorkor may never reach their full growth and height potential. If treatment comes too late, a child may have permanent physical and mental disabilities.
If left untreated, the condition can lead to coma, shock, or death.The condition also makes a person more vulnerable to infection, which, alongside a weakened immune system, can lead to life threatening complications.
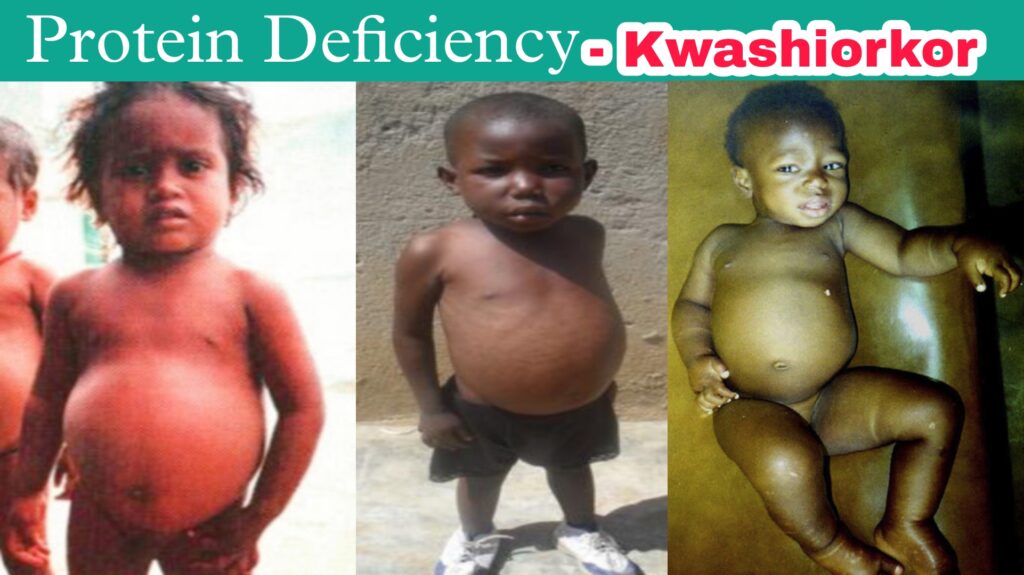
Symptoms of kwashiorkor – Children with kwashiorkor often have very little body fat, but this is not always the case.
Edema can mask how little body weight a child has. The child may appear to be a typical weight or even plump, but this appearance is swelling due to fluid, not the presence of fat or muscle.Symptoms may include:-
- changes in the color of the hair, which may appear yellow or orange
- dehydration
- lack of muscle and fat tissueslethargy and irritability
- dermatosis, or skin lesions that are cracked, flaky, patchy, depigmented, or have a combination of these characteristics
- loss of appetite
- pitting edema or swelling, usually on the legs and feet, when pressing the skin leaves a finger mark
- frequent skin infections or slow healing wounds,
prevention –
As for the prevention of childhood malnutrition, there needs to be public health changes such as improving agriculture and improving access to healthcare to effectively reduce the rates of malnutrition in children. By educating individuals of childbearing age on proper nutrition and health during and after pregnancy, they can provide their children with the appropriate nutrients from a young age. By ensuring they are equipped with the proper education and resources, caretakers and infants are in better health, ultimately preventing childhood malnutrition.
Because edema can hide decreased muscle mass, it can be hard to diagnose kwashiorkor in young children; however, if cases are overlooked, children become more susceptible to infections and can ultimately lead to morbidity and mortality.
To prevent this from happening, parents can be educated on proper nutrition and the importance of breastfeeding infants to ensure they receive all the nutrients they need. A diet rich in carbohydrates, fats that make up 10% of the total caloric needs, and proteins that make up 15% of the caloric needs can prevent kwashiorkor.
Proteins can be found in the following foods –
Seafood,
Peas,
Nuts,
Seeds,
Eggs,
Lean meat,
Beans,
Diagnosis – When diagnosing kwashiorkor in a child, doctors begin by taking a medical history and performing a physical examination.
They will look for the characteristic skin lesions or rash, as well as edema on the legs, feet, and, sometimes, the face and arms. They will also measure how the child’s weight relates to their height.
In some cases, the doctor may order blood testing for electrolyte levels, creatinine, total protein, and prealbumin.
Typically, however, it is possible to diagnose kwashiorkor from a child’s physical symptoms and a description of their diet.
Children with kwashiorkor tend to have low blood sugar levels, as well as low levels of protein, sodium, zinc, and magnesium.
Thanks!!